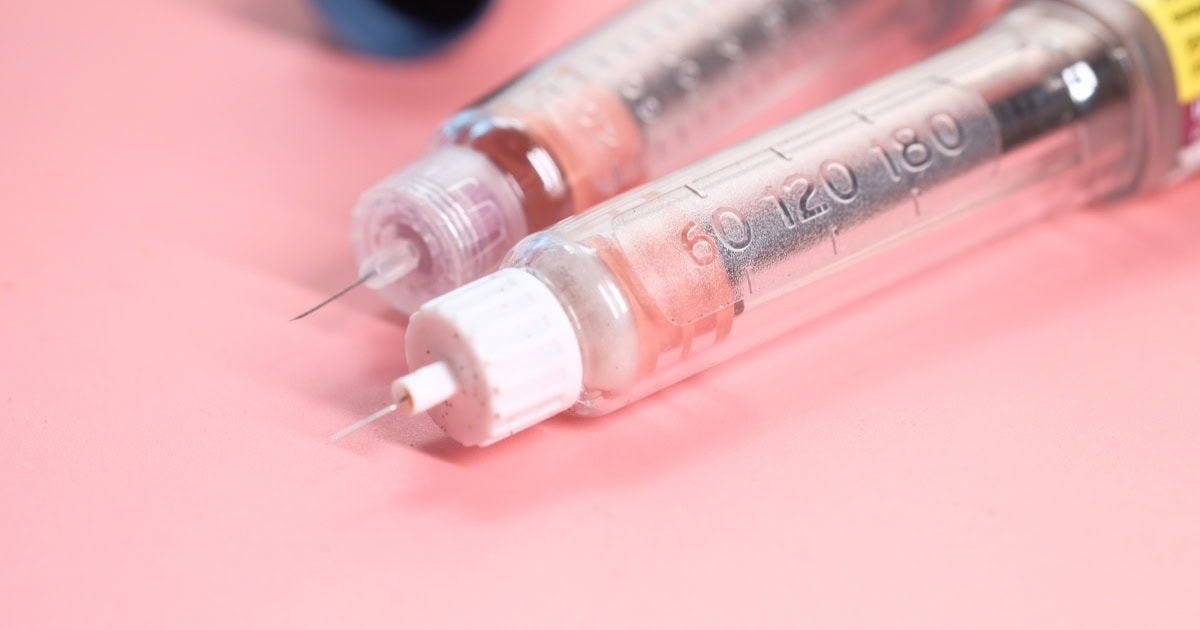
All people with type 1 diabetes need insulin to survive, and millions of people diagnosed with type 2 diabetes need insulin to control their blood sugar levels.
However, insulin is not without side effects. One of the most common concerns expressed by people who use insulin is that insulin tends to cause weight gain.
Achieving and maintaining a healthy weight is important for people with diabetes, so let’s discuss why this happens and what you can do about it.
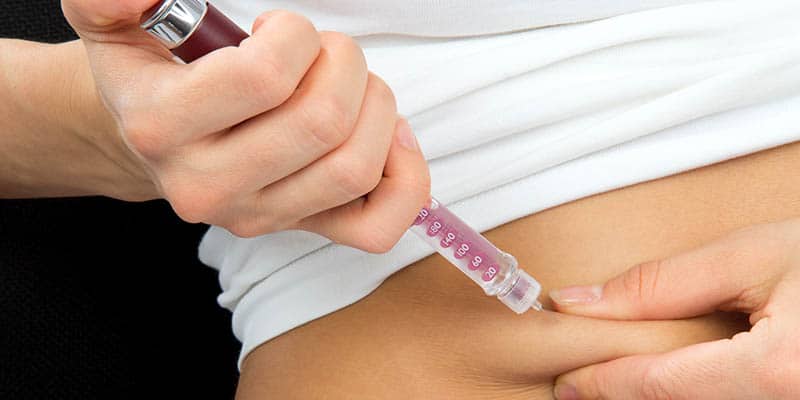
Does insulin cause weight gain?
Insulin is a hormone that facilitates the uptake of sugar (glucose) by nearly every cell in the body, including muscles, liver, and fat cells.
Our cells burn glucose for fuel all the time. When our fuel intake (calories in) is greater than our energy expenditure (calories expended), we tend to store more glucose than we expend.
Muscle cells and liver cells store this excess glucose in a form called “glycogen.” Glycogen is a very dense and compact form of glucose. Fat cells store excess glucose as fat.
Starting insulin therapy can lead to weight gain for several reasons.
- Improved glucose absorption
Before starting insulin therapy, high blood sugar levels often mean that the body is not absorbing nutrients efficiently. When insulin helps glucose enter cells, the body retains more calories, sometimes leading to weight gain. - Reduced glycosuria (loss of sugar in the urine)
When there is a lack of insulin, excess glucose leaks into the urine. This calorie loss stops when insulin controls blood sugar levels. result? More calories remain in the body. - increased appetite
Insulin can sometimes trigger hunger signals. If not carefully managed, it can lead to overeating. - hypoglycemia and overeating
Hypoglycemia (a side effect of insulin therapy) often causes people to take in extra calories to stabilize blood sugar levels, which can increase over time.
When insulin therapy is started and blood sugar levels fall to normal levels, excessive urination and loss of glucose in the urine stops. Our cells resume storing all food in the form of fat or glycogen, and our weight returns to a level appropriate for food intake and calorie expenditure.
In other words, insulin itself does not cause weight gain. It simply restores healthy blood sugar levels and allows you to meter out the amount you need based on your eating and exercise patterns.
What is the average weight gain due to insulin?
Studies have shown that the average person with type 2 diabetes gains up to 3 pounds (1.4 kg) during the first year of insulin use, and 10% gain more than 5 pounds (2.3 kg).
The Diabetes Control and Complications Trial (DCCT) found that type 1 patients who received intensive insulin treatment gained 10 pounds (4.5 kg) more weight than patients who used less insulin. However, this weight gain disappears in long-term follow-up.
Is there any point in using insulin if it only makes you gain weight?
If you have type 1 diabetes or have reduced insulin production, you need to take insulin to survive. You have no choice.
Insulin is also the most effective way to lower blood sugar levels to normal levels, and normal blood sugar levels are essential for making lifestyle changes that will ultimately help you lose body fat and maintain a healthy weight.
When blood sugar levels rise, people tend to feel tired and lethargic. It’s not easy to exercise when you feel that way! Lowering blood sugar levels restores your energy, giving you the strength and posture to maintain an active lifestyle.
High blood sugar levels may make you feel hungry. By keeping your blood sugar levels close to normal, you can better control your food intake, especially your intake of high-calorie sweets and other snacks.
In other words, if you gain a little today, you will lose a lot tomorrow.
How to stop insulin weight gain
Accept the fact that you will tend to gain some initial weight due to insulin use and lower blood sugar levels. So how can you avoid getting too much? Here are some ideas:
avoid hypoglycemia (hypoglycemia)
If you have experienced Any If you have hypoglycemia (usually defined as a blood sugar level below 70 mg/dl), talk to your health care team about reducing the amount of insulin that works during hypoglycemia.
Similarly, if you need to eat; prevent If your blood sugar levels are low, you may be taking too much insulin.
Hypoglycemia not only means you need to eat foods you wouldn’t normally consume, but it also means your blood sugar levels are low. excess insulin – Taking in more insulin than your body needs. Excess insulin promotes the accumulation of fat stores and excessive weight gain.
Reduce insulin dose whenever possible
Similarly, look for any opportunity to reduce your insulin requirements. Reducing your carbohydrate intake is one way to accomplish this.
A good place to start is to eliminate drinks containing carbohydrates. The same goes for reducing snacking.
When eating, reduce your intake of carbohydrate-rich foods such as potatoes, rice, bread, pasta, and cereals. Instead, increase your intake of red meat and low-starchy vegetables.
improve your eating habits
Improving your diet will always help you lose weight and manage your weight, whether you are using insulin therapy or not.
The American Diabetes Association recommends a basic diet that includes:
- Use low-starchy vegetables as the base of your plate
- Lean protein and plant-based protein sources
- High-quality carbohydrates such as starchy vegetables, fruits, whole grains, and low-fat milk
- Low amount of added sugar
- healthy fats
- reduce processed foods
- water or zero calorie beverage
A diabetes-friendly diet rich in fiber and protein and low in refined carbohydrates reduces the amount of insulin needed and makes weight management easier.
exercise
Physical activity can also help lower insulin requirements by increasing insulin action. Walking extra throughout the day may help reduce your dose of long-acting (or “basal”) insulin.
Moderate exercise after meals can significantly reduce the amount of fast-acting (“bolus”) insulin at mealtimes. Talk to your health care team about these adjustments.
Try to reduce stress
Also, look for ways to lower your stress levels. Emotional stress makes your body resistant to insulin.
Learning how to relax can go a long way in reducing your need for insulin. It also helps you get into the right mindset to eat and exercise in a healthy way.
adjust your lifestyle
Reducing stress, physical activity, and a healthy diet can all help you lose weight. And when you lose weight, insulin works better.
When insulin works better, you need less insulin and can lose more weight. What a beautiful cycle!
One of the best ways to start on the path to a healthier lifestyle is to consult a registered dietitian with expertise in both diabetes and weight management. Meal planning guidance and education have been shown to reduce insulin-related weight gain.
treat wisely
When using long-acting insulins, 24-hour “basal” insulins tend to cause less weight gain than intermediate-acting insulins such as NPH.
Also, using 24-hour basal insulin tends to result in less hypoglycemia, which, as mentioned above, is beneficial in terms of weight loss.
Using an insulin pump can also eliminate unnecessary insulin doses, typically reducing total insulin use by 10-20% and improving blood sugar control.
Many people take another diabetes drug along with their insulin to reduce the required dose or to lose weight.
Insulin sensitizers, such as rosiglitazone and pioglitazone, can help reduce insulin requirements.
Metformin reduces the body’s natural secretion of glucose into the bloodstream, which may also reduce the need for insulin.
Pramlintide, an injectable drug, helps slow digestion, blunt appetite, and block glucagon secretion, often reducing insulin requirements at mealtimes.
Also, another injectable drug, exenatide, can help improve insulin sensitivity and increase the body’s own insulin production after meals.
Consider GLP-1
GLP-1 drugs such as semaglutide (Ozempic) and tirzepatide (Mounjaro) have proven to be highly effective weight loss drugs. Ask your doctor if these medications are the right option for you.