PCOS and diabetes are primarily linked due to common hormonal and metabolic changes. Here’s how to manage both conditions at the same time and reduce long-term risk.
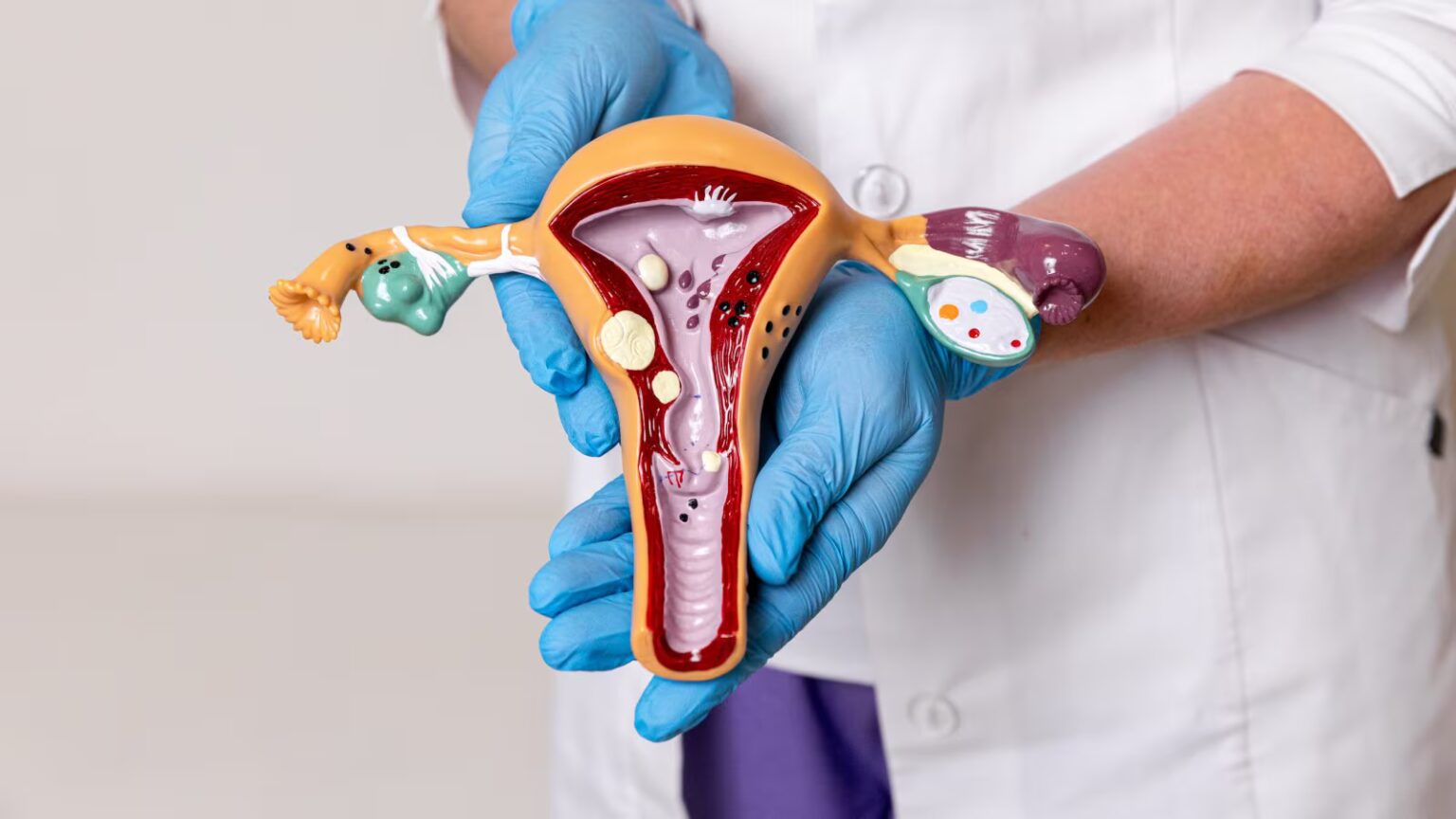
Polycystic ovary syndrome (PCOS) is a hormonal disorder in which small fluid-filled sacs, or cysts, form in the ovaries. It often causes irregular periods and is one of the most common causes of infertility, affecting approximately 5 million women worldwide. According to the U.S. Centers for Disease Control and Prevention, more than half of women with PCOS will develop type 2 diabetes by age 40. In India, almost one in five women of reproductive age has PCOS, which is higher than in many other countries. Experts point to increased stress, sedentary habits, and environmental pollution as the main causes. However, many cases remain undiagnosed due to low awareness. What many people don’t realize is that PCOS and diabetes (one a hormonal disease, the other a metabolic disease) are deeply connected. Understanding this connection is key to protecting your long-term health.
Hormone metabolic relationship between PCOS and diabetes
PCOS is one of the most common hormonal disorders in young women, and the strongest association with diabetes is caused by insulin resistance. Dr Sudeshna Ray, Senior Consultant Gynecologist and Obstetrician at Jaslok Hospital, explains that in PCOS, the body does not respond properly to insulin. To compensate, the pancreas produces more insulin. This is known as hyperinsulinemia.
This excess insulin causes the ovaries to release high levels of androgens (male hormones such as testosterone). This causes typical PCOS symptoms such as irregular periods, acne, weight gain, and unwanted facial hair. However, over time, blood sugar levels also rise, increasing the risk of prediabetes and type 2 diabetes.
A 2024 study published in the Journal of Ovarian Research also strengthens this link, finding that insulin resistance appears nearly two to three times earlier in young women with PCOS than in women without PCOS.
PCOS increases diabetes risk even without weight gain
A common misconception is that only overweight women with PCOS develop diabetes. However, Dr. Ray emphasizes that even thin women can have insulin resistance. The problem isn’t just fat storage, but also how the body’s cells respond to insulin. This is why regular screening is essential for all women with PCOS, regardless of body type. Early detection can prevent future complications.

PCOS and Type 1 Diabetes: Links
Research shows that women with type 1 diabetes can also develop PCOS-like symptoms. People who require higher doses of insulin often exhibit signs such as irregular cycles and excessive hair growth. This overlap reveals how closely related reproductive hormones are to insulin levels. Recognizing this link will allow doctors to more effectively treat both conditions and personalize care for women managing type 1 diabetes, according to Dr. Ray.
How does PCOS cause a diabetic cycle?
When insulin stops working efficiently, the following happens:
- Glucose remains in the blood without being used for energy.
- This gradually leads to prediabetes and type 2 diabetes.
- High insulin causes the ovaries to produce more male hormones, worsening PCOS symptoms.
- Excess insulin promotes fat gain, increases inflammation, and changes cholesterol levels. All of these increase your risk of diabetes.
If PCOS-related insulin resistance is not managed, it can also cause symptoms such as:
How can I manage PCOS with diabetes?
Both symptoms have the same root cause: insulin resistance. So addressing this will help you manage both. Here are six important tips to manage it.
1. Maintain a healthy weight. Even a 5 to 10 percent weight loss can improve insulin sensitivity and regulate your cycle.
2. Choose balanced, whole foods. Eat more fruits, vegetables, whole grains, lean proteins, and healthy fats. Minimize sweet foods and refined carbohydrates that spike blood sugar levels.
3. Move your body every day. A combination of walking, strength training, and aerobic exercise is the most effective way to improve insulin sensitivity.
4. Get regular health checkups. Regular testing of blood sugar levels and hormones can help detect problems early.
5. Medical support if needed: Your doctor may recommend medications such as metformin to manage symptoms of insulin resistance and PCOS.
6. Prioritize sleep and stress control: Lack of sleep and chronic stress worsen hormonal balance. Yoga, meditation, or simple breathing exercises can help.
Dr. Ray suggests that both conditions can be effectively managed with early screening, lifestyle changes, and proper medical guidance.